Clea Simon
Harvard Correspondent
The Monk Skin Tone scale, devised in 2019 by Professor Ellis Monk, helps create more accurate medical diagnostic tools for patients with dark skin
/ Read time: 7 minutes
Harvard Correspondent

A two-dollar badge is saving lives in hospitals around the world. The product, groundbreaking but simple, is a scale of colors that reflects a more complete range of human skin tones.
Developed by Professor of Sociology Ellis Monk, the Monk Skin Tone (MST) was inspired by a 2019 discussion with Monk’s then-pregnant wife. A Brazilian, she pushed her husband to consider the huge range of skin tones in the ethnically diverse United States and her home country. The MST went on to take commercial technology by storm. Now the scale is making medical technologies more accurate, protecting human health at very low cost.
The previous standard for measuring skin tone was the Fitzpatrick scale. Developed by the late Harvard Medical School dermatologist Thomas B. Fitzpatrick in 1975 to measure ultraviolet reactivity, it was intended to judge skin cancer risk in light-skinned people. Although the scale was expanded from its original four points to include two points for “brown” and “Black” skin, its resulting six points still fell far short of the full range of human melanin.
The idea of an improved scale had been “latent for years,” said Monk, whose colleagues pointed to his work with colorism in encouraging him. The sociologist ended up developing a 10-tone, open-source scale aimed at improving inclusivity in skin tone classification across technological and clinical domains.
Its original form, with colored spheres, reflected a much wider range of skin tones. But Monk settled on a 10-point scale for pragmatic reasons. “Ten points are pretty much the breaking point for having people be able to consistently use it as a subjective scale,” he said.
At the time, the tech industry was riddled with shortcomings concerning skin tone. As Monk pointed out, if you typed “cute babies” into most search engines six years ago, “you got a bunch of white, blonde, blue-eyed babies.”
“To fix that problem,” he continued, “you need an image search engine that properly tags things by color and allows people on the engineering side to create more fair search representation essentially.”

Google adopted the MST scale in 2020. It has since improved the accuracy of technologies ranging from cameras to self-driving cars, all of which previously struggled with recognizing the faces of people of color.
“The scale has really become infrastructure for fairness, infrastructure for representation,” Monk said.
The same year that Monk launched the scale with Google, he was awarded the National Institutes of Health Director’s New Innovator Award. Monk was the first sociologist to win this $2.5 million grant, though it was terminated in 2025. Nevertheless, the funding prompted Monk to launch a project on pulse oximetry that has already proved transformative.
Monk collaborated with Robert Wilson, a professor of electro-optics and photonics at the University of Dayton, who happens to be Monk’s high school friend. He’s “an expert in optics and how light propagates through flesh,” Monk explained.
Working with the Open Oximetry Project at the University of California, San Francisco, Monk and Wilson tackled a deadly problem. Pulse oximeters measure blood oxygen by analyzing light as it passes through the skin via a small finger clamp. However, darker skin absorbs light differently than lighter skin. Because pulse oximeters originally used white skin as the standard, people with darker skin would get inaccurate readings. And because these inaccurate readings skewed higher, many people with dangerously low blood oxygen ended up with too-high readings, meaning they would appear to have normal blood oxygen.
“This was huge during COVID,” said Monk, citing a 2020 study in the New England Journal of Medicine that documented overestimates of oxygen saturation by roughly 3 to 4 percent on dark-skinned patients. In practice, this could mean a reading of 95 percent, which is considered healthy, Monk pointed out. “But you could really be at 89 percent,” which is dangerously low.
“That’s where the delayed treatment or no treatment comes in and it disproportionately affects anyone with darker skin,” said Monk, noting the factor likely contributed to higher rates of death among people of color during COVID-19. “It’s colorism baked into the device.”
By 2021, the FDA was writing about these inaccuracies, recommending a study incorporating the MST scale. The FDA’s January 2025 draft guidance, co-authored by Monk, named the MST as the skin tone measurement tool for pulse oximeter premarket evaluation.
Early this year, the largest independent pulse oximeter study ever conducted tested 34 devices on 155 participants across 30,174 paired samples. Only 1 of 34 passed the FDA’s anticipated criteria. Monk was also a co-author of that study, which used the MST as the measurement infrastructure that proved the devices were faulty.
Since 2024, the MST has been named in two International Organization for Standardization (ISO) recommendations for devices gathering biometrics and measuring pulse oximetry. Now oximeter manufacturers, such as Medtronic, have started to incorporate the MST scale.
The MST has seen additional life-saving applications. For example, each year, hospital-acquired pressure injuries (HAPIs), such as bedsores, cause roughly 60,000 deaths in the United States and cost $26.8 billion. The injuries are traditionally under-diagnosed in darker-skinned people, but a laminated badge displaying the MST scale, along with 15 minutes of training, is helping nurses recognize more incidents of HAPIs. A 2026 study finds the badge, which costs approximately $2, reducing these injuries by 94 percent at a 900-bed Level I trauma hospital in Los Angeles.
A similar badge, called the “bili-ruler,” is also being used to measure jaundice caused by an excess of bilirubin in newborns. This neonatal jaundice can cause permanent brain damage or death. However, in darker-skinned people, it commonly goes unnoticed.
“People just look at you and go, ‘Oh, are you getting yellow?’” Monk explained. “Good luck detecting that on darker skin until it’s too late.”
Now, the bili-ruler, which costs roughly $9, allows healthcare professionals to judge levels of jaundice against a full range of skin colors. In western Kenya, where the bili-ruler has been in use since January 2025, there have been zero jaundice-related deaths among 930 screened infants, according to the Gates Foundation’s PRISMA Maternal and Newborn Health Study conducted at six health facilities.
A further Gates Foundation-funded protocol is now being used to screen 5,400 infants using the ruler in Ghana, India, Pakistan, Kenya, and Zambia — the largest multi-country clinical deployment of a skin tone standard in history.
As William Julius Wilson, the Lewis P. and Linda L. Geyser University Professor Emeritus, pointed out, Monk’s scale has “crossed into some pretty unexpected territory — healthcare, computer science, photography, and AI.”
“The results speak for themselves,” Wilson added. Referring to the adoption of the MST to diagnose HAPIs, he said, “These kinds of injuries hit darker-skinned patients the hardest, so Monk’s nurse training program is making a real difference in how they’re spotted and treated.”
But medical uses of the MST are only just beginning, as was noted in a recent article in Nature discussing its use in dermatology. Despite termination of his NIH grant, Monk intends to continue this work, having seen applications for common medical tests such as EKGs and EEGs, which also take measurements through the skin.
“People have been operating blind to color,” he said. “You can’t do that, because the skin is your interface with the technological world.”

At Harvard, drummer Raghav Mehrotra ’26 built knowledge about the music industry — and a sizable social media following.
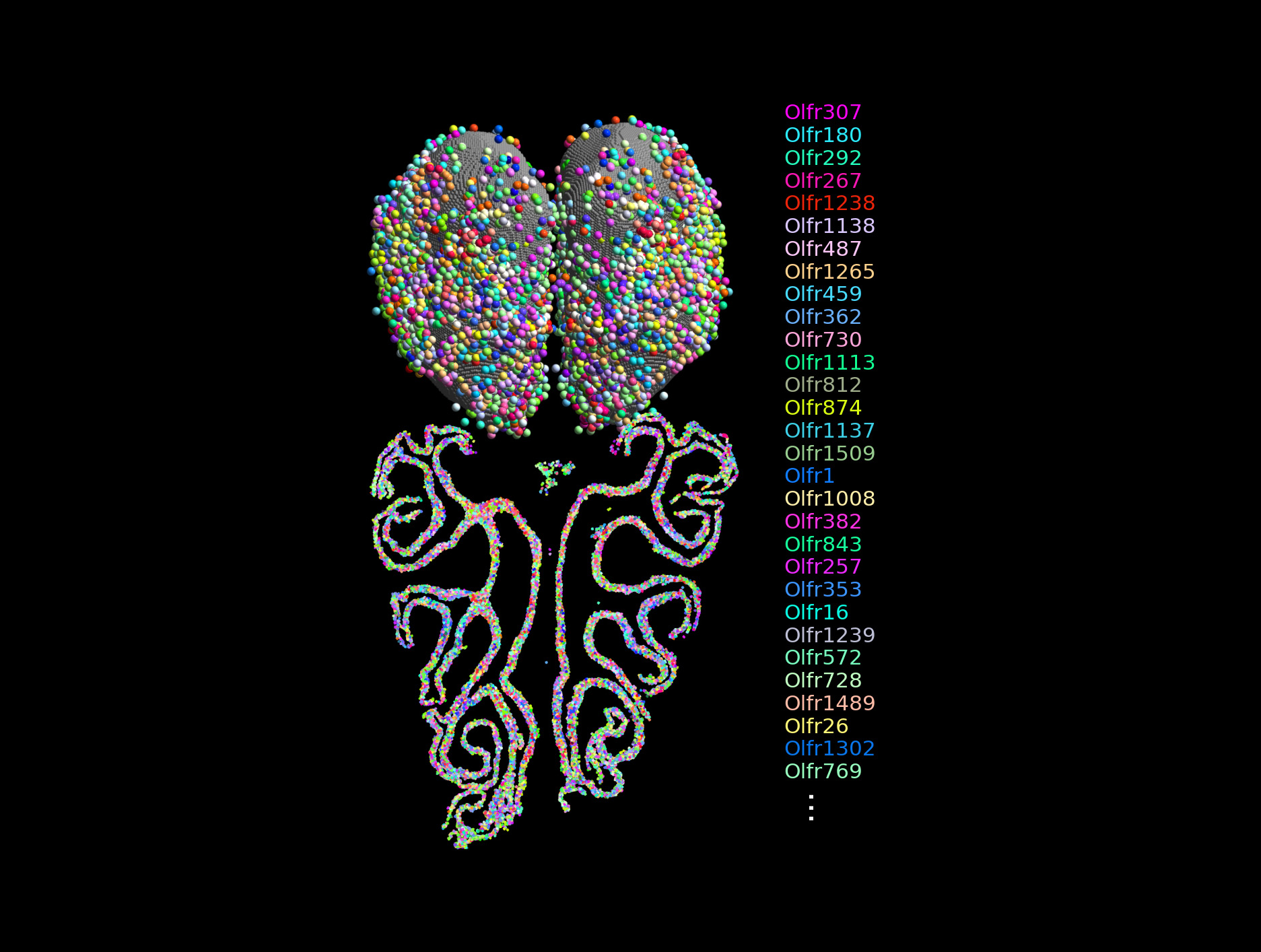
A team of researchers from two labs has created the most comprehensive map to date of how the primary olfactory system detects and organizes social and predator odors.

A few months shy of 30, Richard Glazunov is poised to graduate from Harvard College with a degree in government.